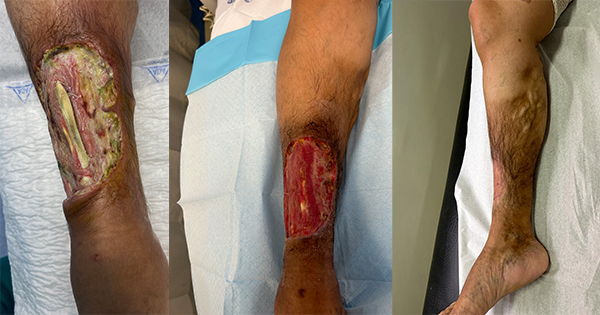
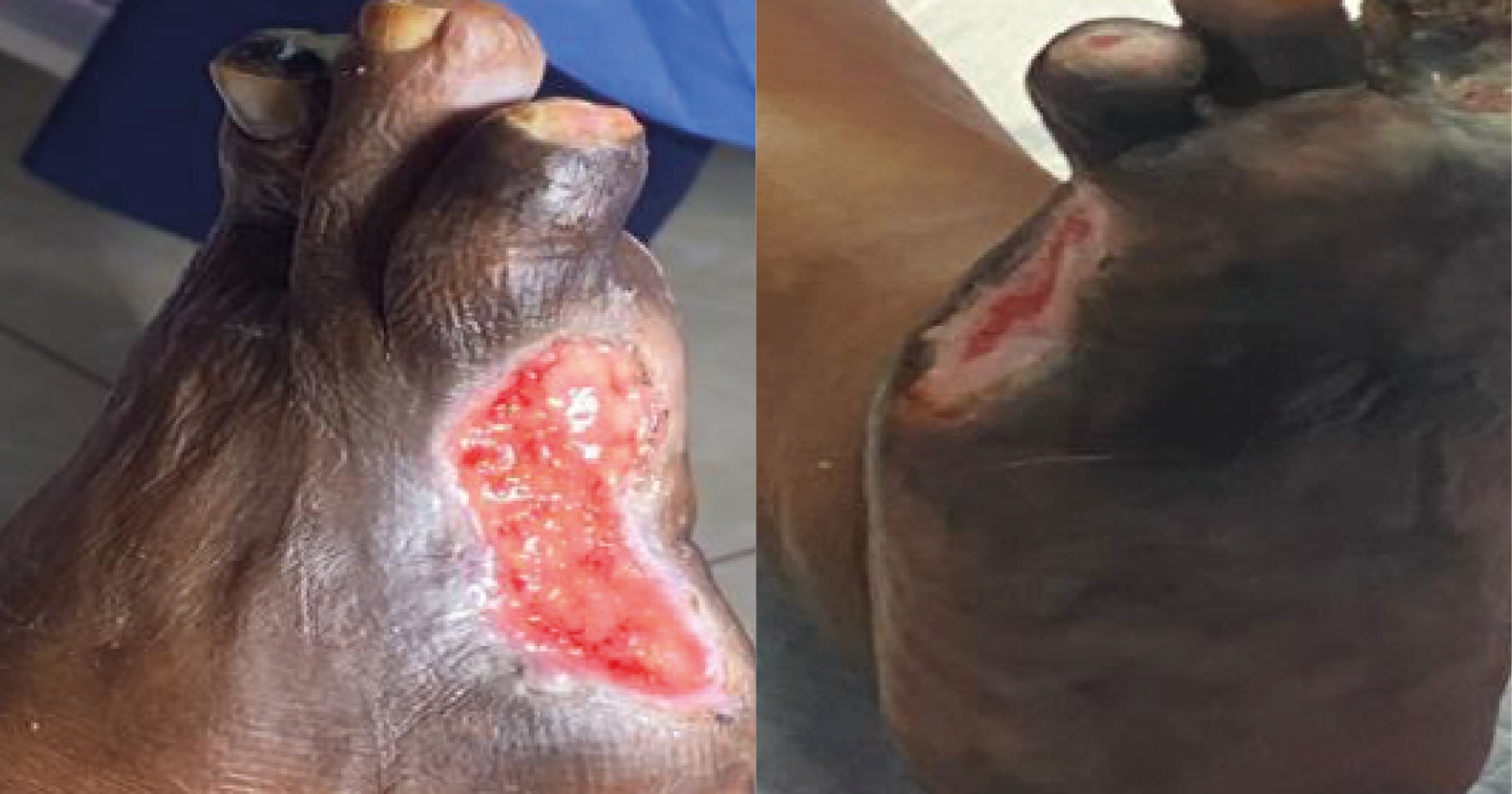
<p>This article describes the latest significant research concerning wound infection and the effect this has had on the day-to-day practice in a regional hospital in Australia. The author highlights the importance of tackling biofilms when dealing with chronic wound infection and the need to standardise swabbing techniques. The author also outlines the impact that wound care research has had on her personal vision of wound care.</p>