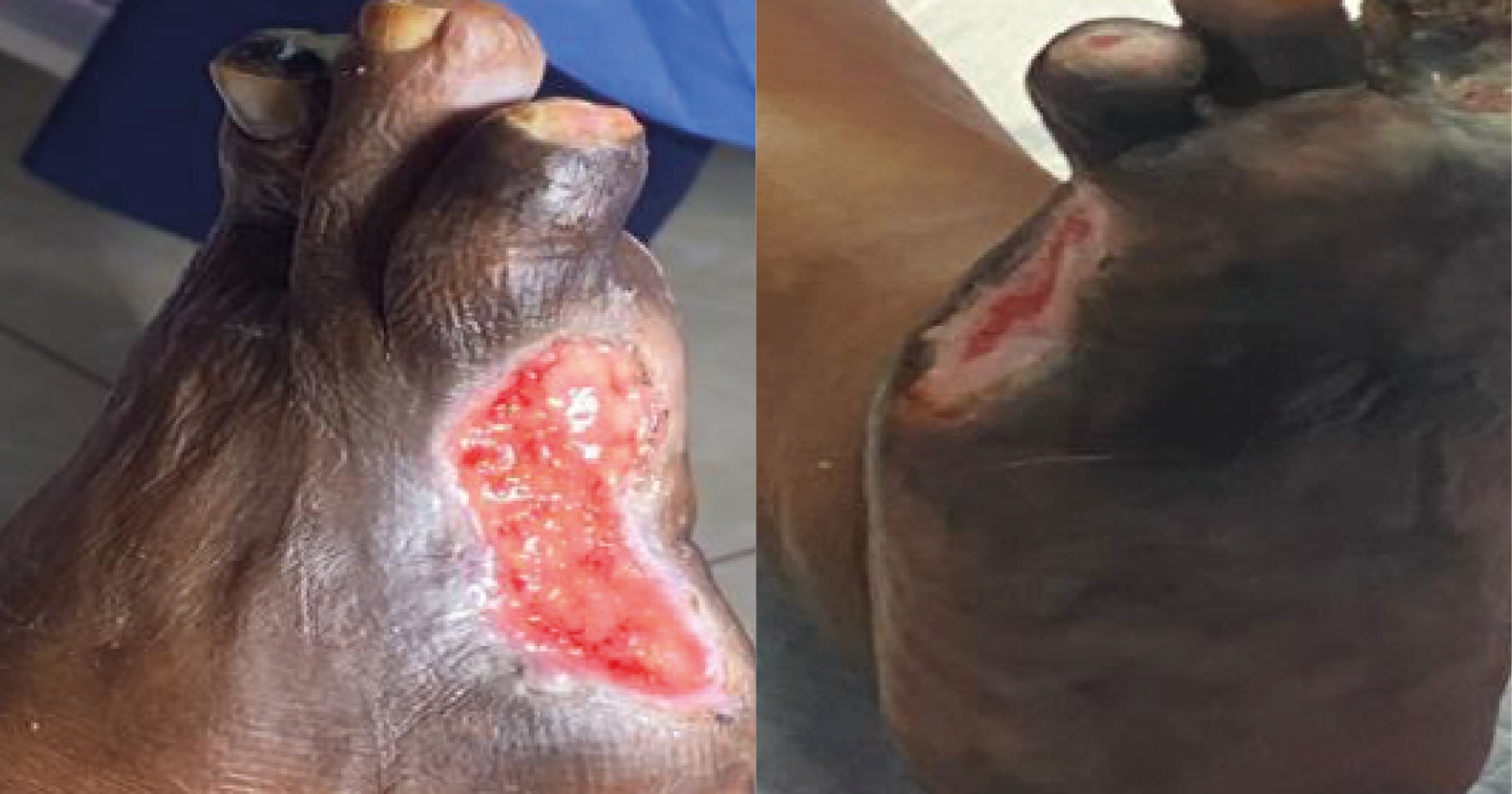
<p>Debridement of non-viable tissue from any wound is an accepted principle of wound care and is primarily aimed at achieving wound healing. However, a 2010 consensus document highlighted the fact that many clinicians undertake this process without adequate knowledge or preparation: 'Upskilling practitioners in the most recent advances in debridement tools and techniques will help to ensure that the appropriate and optimum treatment options are implemented, thus improving patient care and clinical outcomes'[1].</p>